Can tooth bleaching reduce plaque and gingivitis? A systematic review.
Lorenzo Breschi
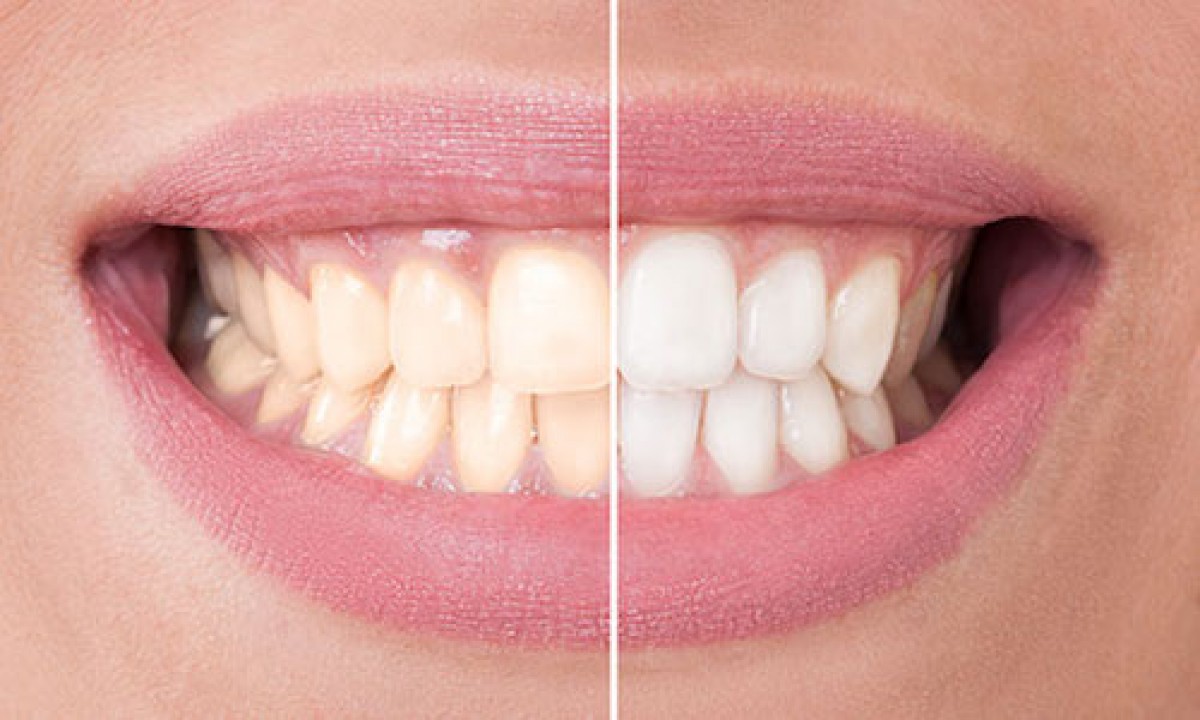
Aesthetics is becoming everyday more and more important for patients. Indeed, one of the main reason for a dental consultation is the alteration of tooth appearance. Changes in color could be pathological, such as color modifications in non-vital teeth, fluorosis or tetracycline induced discoloration, or non-pathological, due to the natural laying down of secondary dentine, resulting in a gradual darkening of teeth with age. In order to improve teeth appearance, two bleaching agents are mostly employed: hydrogen peroxide and carbamide peroxide. The two materials are both relatively safe and effective, although some side effects could occur. Different side effects have been described after tooth bleaching depending on the formulation, concentration and application mode, especially after the massive distribution of the “at home” formulations, directly sold to the consumer without supervision or control of a qualified professional.
Problems were reported in literature on hard and soft tissues, but also on the quality and concentration oral bacteria. In particular, the modification of the bacterial flora presented controversial considerations: on the one hand, it seems that plaque formation could be negatively affected by the increase surface roughness after bleaching, on the other hand, some in vitro studies showed that bleaching products could have potential antibacterial properties due to the oxygen release and the formation of reactive oxygen species.
Being evident the need to evaluate the effect of bleaching agents on oral biofilm, as well as on plaque formation and gingivitis levels at short term and a long term, Sanz-Sánchez and his team published in 2019 a systematic review on the topic with the purpose of assessing the effects of different products used for tooth bleaching in the changes of plaque and gingivitis indices in comparison with a control group (no treatment or placebo).
MATERIALS AND METHODS
In the above mentioned manuscript, two electronic databases were used as sources for the research. The inclusion criteria were patients without periodontitis and over the age of 18 years treated with tooth-whitening products containing hydrogen peroxide or carbamide peroxide. The electronic search delivered 382 titles. After their evaluation seven studies were included, and six were used in the meta-analysis.
RESULTS
The result of this research showed a statistically significant greater reduction in plaque formation and gingivitis index during treatment in the test group when compared to the control group. In some studies, however, it has been showed that, after tooth bleaching, teeth could be more prompt to plaque accumulation due to surface modifications. Enamel surface alterations may vary according to the whitening products used and seem to be associated with the use of bleaching agents with a low pH. Therefore, bleaching products should ideally have a neutral pH to minimize the risk of a potential damage. The pH values of the bleaching agents range between 4.5 and 10.8, showing that some of the products on the market are below the critical point of enamel demineralization (pH 5.5). Indeed, the demineralization process seems to be mainly correlated to the low pH instead of the presence of the hydrogen peroxide itself. Therefore, with the available data, it is difficult to validate the hypothesis that tooth-whitening products could lead to an increase in plaque formation at long term due to an increase in enamel roughness.
The relevance of this topic should not be forgotten. The increased demand for cosmetic dental treatment from the population has favored the overgrowth of dental whitening requests, even without professional supervision. In the United States of America, 34% of the adult population reported being unsatisfied with the current color of their teeth, and in a survey of 3215 subjects in the United Kingdom, 50% of the respondents perceived some degree of discoloration. The safety and efficacy of the products used for this treatment have been demonstrated in several studies but in any case, bleaching products should not be applied without professional supervision and patients undergoing treatment should attend the follow-up visits to control tissues and oral health during the treatment.
CONCLUSIONS
The authors concluded that, within the limitations of the systematic review, the use of tooth‐whitening products is associated with a statistically significant reduction in the levels of dental plaque and gingivitis during treatment. However, no data are available to confirm these findings in a long-term basis and to support that these changes are clinically relevant. Nevertheless, it is important to maintain good oral hygiene levels before, during and after treatment.
For additional informations:
Changes in plaque and gingivitis levels after tooth bleaching: A systematic review
 Related articles
Related articles
Periodontology 30 April 2026
The remit of this working group was to update the existing knowledge base in non-surgical periodontal therapy.
Periodontology 15 April 2026
Topical administration of simvastatin recovers alveolar bone loss in rats
Simvastatin, a cholesterol-lowering drug, has been reported to show anabolic effects on bone metabolism.
Periodontology 13 March 2026
Diagnostic measures for monitoring and follow‐up in periodontology and implant dentistry
This review discusses the role of diagnostic measures in the lifelong management of periodontal disease and peri-implant complications.
Periodontology 01 December 2025
Ceramic abutments--a new era in achieving optimal esthetics in implant dentistry.
In the visible dental region in particular, implant-prosthetic restorations filling single-tooth gaps make exacting demands on function and esthetics.
Periodontology 14 November 2025
This study was carried out to assess the oral hygiene awareness and practices amongst patients visiting the Department of Periodontology at Gian Sagar Dental College and Hospital, Ramnagar (Patiala).
 Read more
Read more
News 07 May 2026
Two-day event in Broomfield, Colorado, brings dental, medical and behavioral health professionals together for hands-on collaboration
News 07 May 2026
My Mountain Mover, the leading provider of Medical Virtual Assistants for healthcare practices across the United States, proudly announces its official expansion into the dental in
Editorials 07 May 2026
Achievements Unlocked: DDS Class of 2024 Student and Faculty Awards Announced
Rick Mediavilla, DDS, FAGD, associate professor and associate dean of admission, student and alumni affairs, had the honor of announcing each of the 79 graduates, their plans follo
Orthodontics 07 May 2026
This peer-reviewed orthodontics article summarizes clinical evidence from PloS one (2026). It focuses on findings that may help dental professionals evaluate treatment decisions, patient outcomes, or...