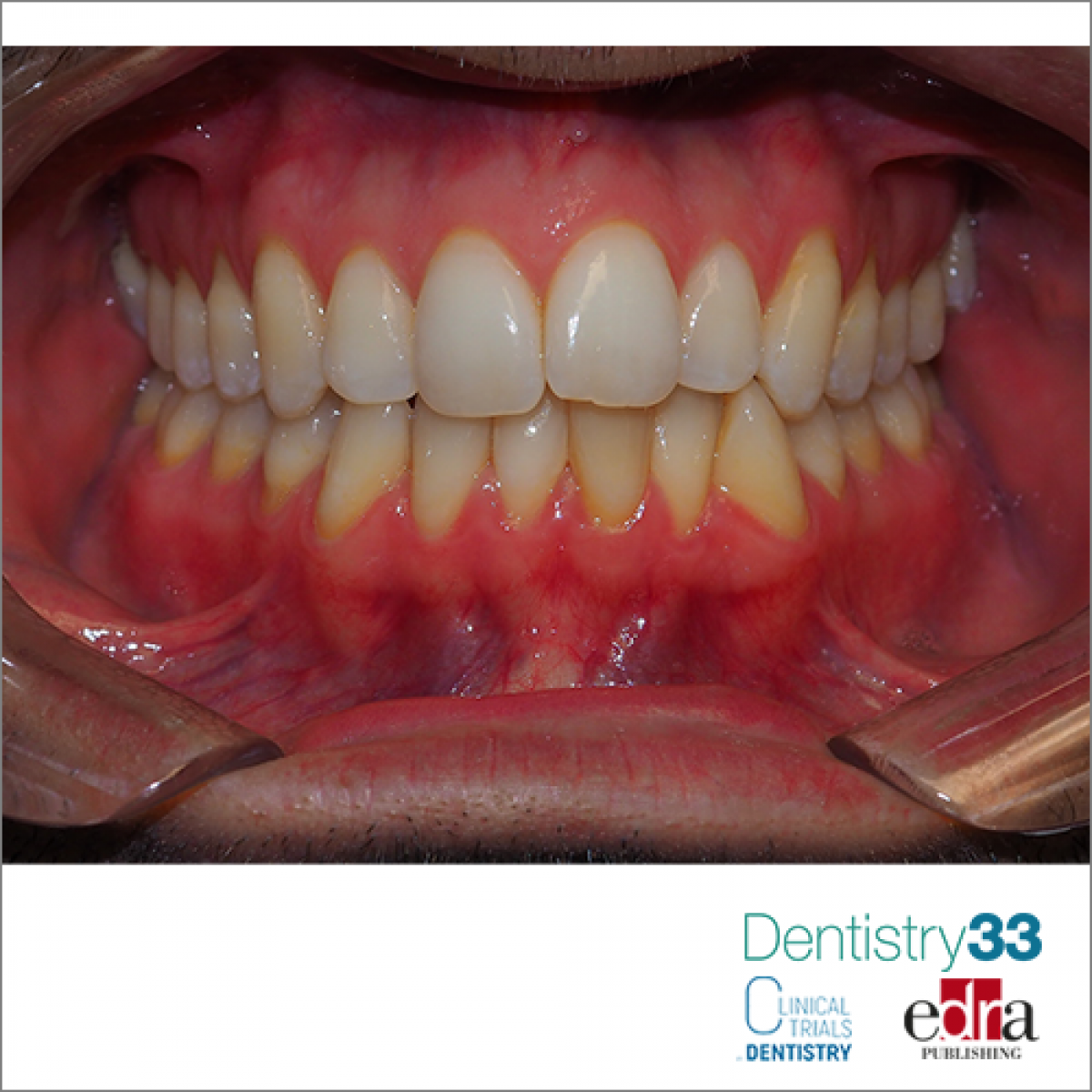
How teeth move during all life
Davide Elsido
Growth-related occlusal changes are well documented in the orthodontic literature and provide essential clinical guidance.
The biologic environment comprised skeletal, dental, and soft tissue and does constantly change throughout its lifetime, even when growth is no longer taking place. In orthodontics, prior understanding of these changes is crucial to design an appropriate treatment plan and to inform the patient regarding the need for posttreatment retention. More importantly, this knowledge can help us understand whether the occurred posttreatment changes are due to the orthodontic intervention or part of the normal developmental or aging process.
Postorthodontic relapse has been attributed to multiple causes, including the reorganization of periodontal and gingival tissues, lack of proper occlusal interdigitation, soft tissue adaptation, oral habits, and growth changes. Because orthodontic treatment alters the normal muscular pattern, it has been suggested that treatment should be limited within the equilibrium zone between intraoral and extraoral muscular forces to prevent relapse because of soft tissue pressure. Anthropological studies suggest that the lack of dental crowding in ancient humans was due to attrition as a consequence of their hard diet. Animal studies have also shown that differences in the hardness of diet are related to significant changes in maxillary width and the presence of rotated or displaced teeth.
Many strategies have been proposed to avoid orthodontic relapse. Lifelong use of bonded retainers is one of the most popular options in an effort to avoid it, and it is currently seen as an inherent part of orthodontic treatment. However, there is no consensus in the literature regarding a predictable retention protocol. Long-term wear of fixed retainers presents a number of disadvantages, such as the need for maintenance, which increases the practitioner’s workload and the costs for the patients, the difficulty to maintain good oral hygiene, the possibility of retainer breakage, bond failure, or accidental activation, which can lead to active tooth movement.
Recently in the AJODO a systematic review was published regarding age-related dental changes in untreated normal human occlusion. The comparative analysis of the included articles aims to serve as a baseline for orthodontic diagnosis and treatment planning.
From the initial 7681 articles founded, 40 were included.
Physiological, occlusal changes because of aging have been reported in humans with normal occlusion.
These can be summarized as follows:
1. Intercanine width increases in the maxillary arch from 3.0 to 13.0 years of age and in the mandibular arch until 8.0 years of age. This is followed by a decrease in mandibular and maxillary arches until 60.0 years of age. Males show larger increases than females, whereas reduction in the mandibular arch from 13.0 to 45.0 years of age is larger than in males than females.
2. Intermolar width increases from 3.0 to 15.0 years of age in mandibular and maxillary arches. In the maxilla, it starts decreasing while the mandible continues increasing until 26.0 years of age. This is followed by a decrease until 42.0 years of age in mandibular and maxillary arches. These changes are larger in males than females.
3. Arch length increases in the maxilla until adolescence and in the mandible until 8.0 years of age. After that, the arch length and perimeter decrease in mandibular and maxillary arches until 60.0 years of age. There are larger changes in the maxillary arch of males, whereas there are larger reductions in the mandibular arch in females.
4. Crowding steadily increases from early permanent dentition until 60.0 years of age. Incisor crowding is greater in the mandibular arch, as well as females.
5. Arch depth increases in mandibular and maxillary arches from 6.0 years of age to adolescence (ie, 13.0 years of age). This change is followed by a reduction until 31.0 years of age.
6. Overjet and overbite increase from 9.0 to 13.0-15.0 years, respectively, followed by a reduction until 20.0 years of age and later a steady increase in overjet until late adulthood.
These changes should be taken into consideration for orthodontic diagnosis and treatment planning. They are also relevant to evaluate the long-term posttreatment results, which is especially important given the increased interest of older age groups in orthodontic treatment.
For additional information: Dental changes in humans with untreated normal occlusion throughout lifetime: A systematic scoping review.
 Related articles
Related articles
Orthodontics 04 June 2026
This peer-reviewed orthodontics article summarizes clinical evidence from PloS one (2026). It focuses on findings that may help dental professionals evaluate treatment decisions, patient outcomes, or...
Orthodontics 21 May 2026
This peer-reviewed orthodontics article summarizes clinical evidence from PloS one (2026). It focuses on findings that may help dental professionals evaluate treatment decisions, patient outcomes, or...
Orthodontics 07 May 2026
This peer-reviewed orthodontics article summarizes clinical evidence from PloS one (2026). It focuses on findings that may help dental professionals evaluate treatment decisions, patient outcomes, or...
Orthodontics 28 April 2026
Esthetic outcomes in orthodontics through digital customization with a lingual appliance system
Contemporary fixed orthodontic appliances are shifting from non-customized pre-adjusted appliances to custom-designed and printed appliances with novel digital setup systems.
Prosthodontics 16 April 2026
The use of orthodontics before fixed prosthodontics in restorative dentistry
For a variety of reasons, orthodontic intervention is often overlooked as a viable modality to correct occlusal, axial, rotational, and space discrepancies before undertaking fixed prosthetic...
 Read more
Read more
New initiative invites dentists to experience DEXIS’ most advanced AI yet, built on scale, speed, and clinical trust.
News 05 June 2026
(Nasdaq: ALGN), a leading global medical device company that designs, manufactures, and sells the Invisalign® System of clear aligners, iTero™ intraoral scanners, and exocad™ CAD/C
News 05 June 2026
(Nasdaq: HSIC), the world’s largest provider of health care solutions to office-based dental and medical practitioners, today announced that its Board of Directors has elected Will
As the University of Colorado School of Dental Medicine celebrates the graduating DDS Class of 2025, we are proud to recognize the students and faculty members whose exceptional de
Oral surgery 05 June 2026
This peer-reviewed oral surgery article summarizes clinical evidence from International journal of oral and maxillofacial surgery (2026). It focuses on findings that may help dental professionals...