Toothwear in a multidisciplinar way
Tooth wear / Tooth surface loss (TSL) is a normal yet irreversible physiological process that occurs throughout life. It is however, considered pathological when the degree of destruction of hard tissue is excessive leading to functional degradation, sensitivity, and aesthetic impairment.
Pathological TSL can be asymptomatic and thus many patients are unaware of the condition. There is general agreement of the multifactorial / complex nature of TSL, yet its treatment is relatively standardised when following certain protocols.
TSL has been described by the following:
1. Attrition: direct tooth-tooth contact
2. Abrasion: sliding / rubbing of abrasive external objects
3. Abfraction: tensile stress generated from non-axial cyclic occlusal forces. A result of flexure and fatigue of enamel / dentine at a location distant from the actual point of loading.
4. Erosion: dissolution of dental hard tissue by non-bacteriogenic acids.
CASE
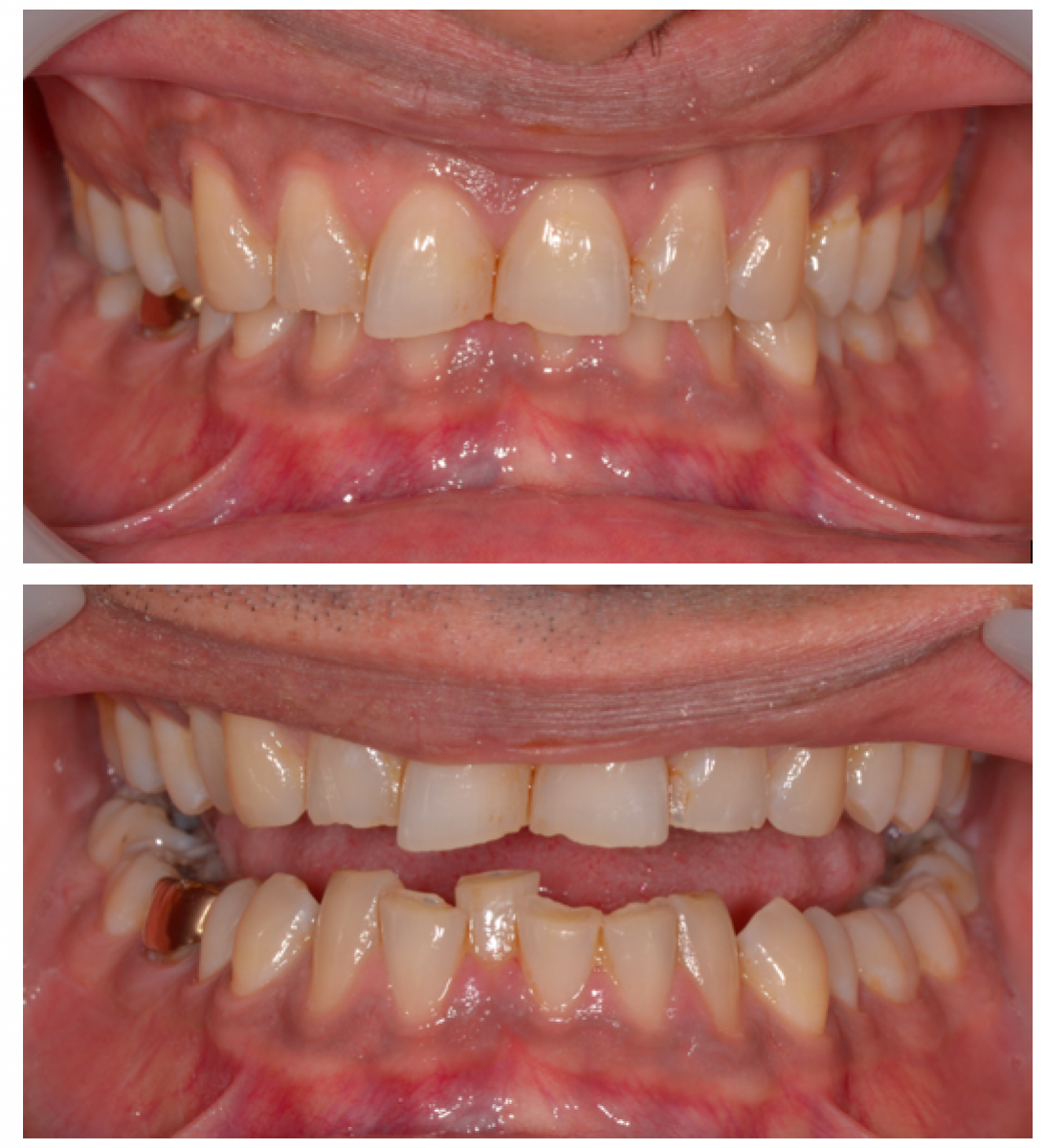
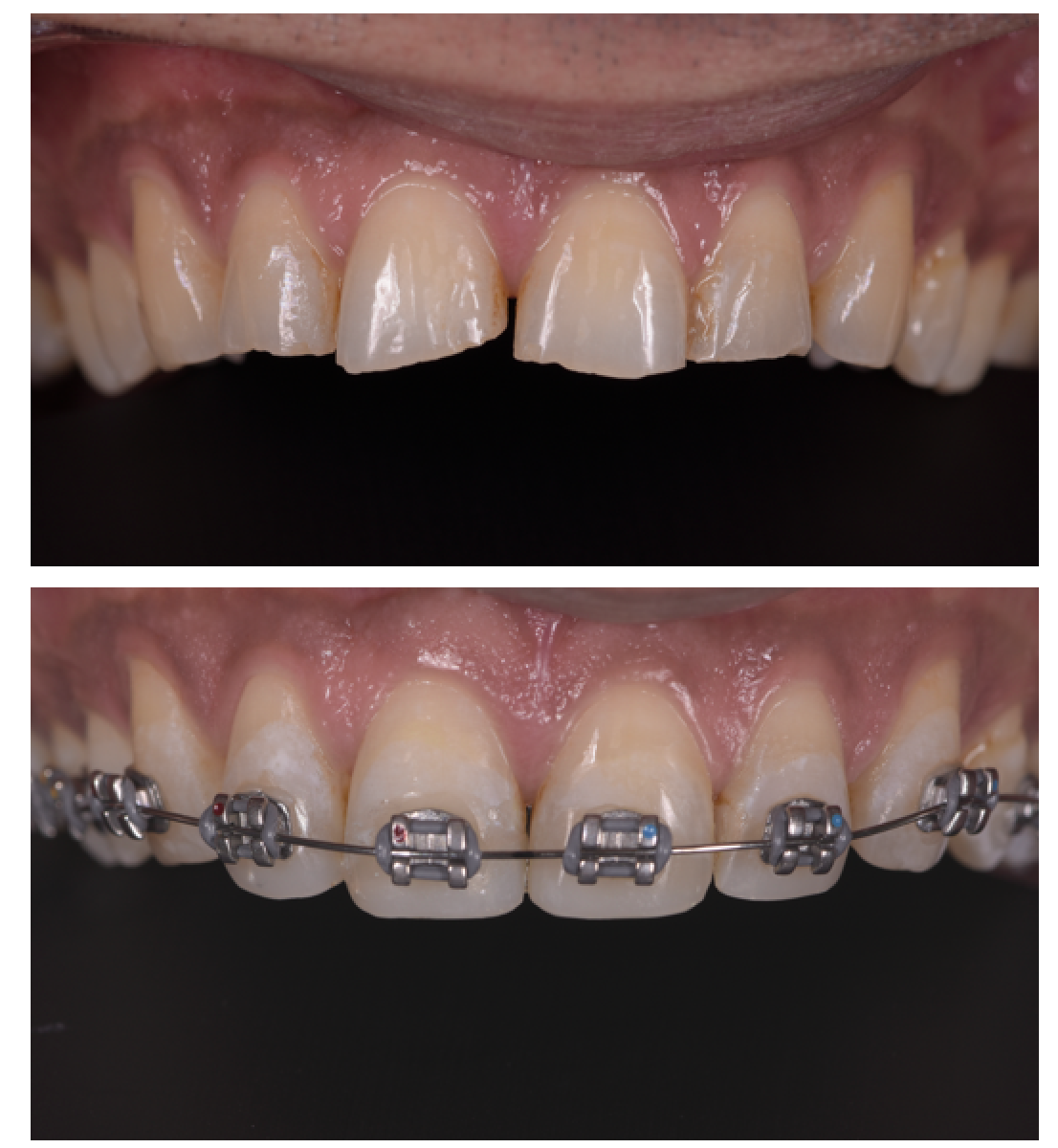
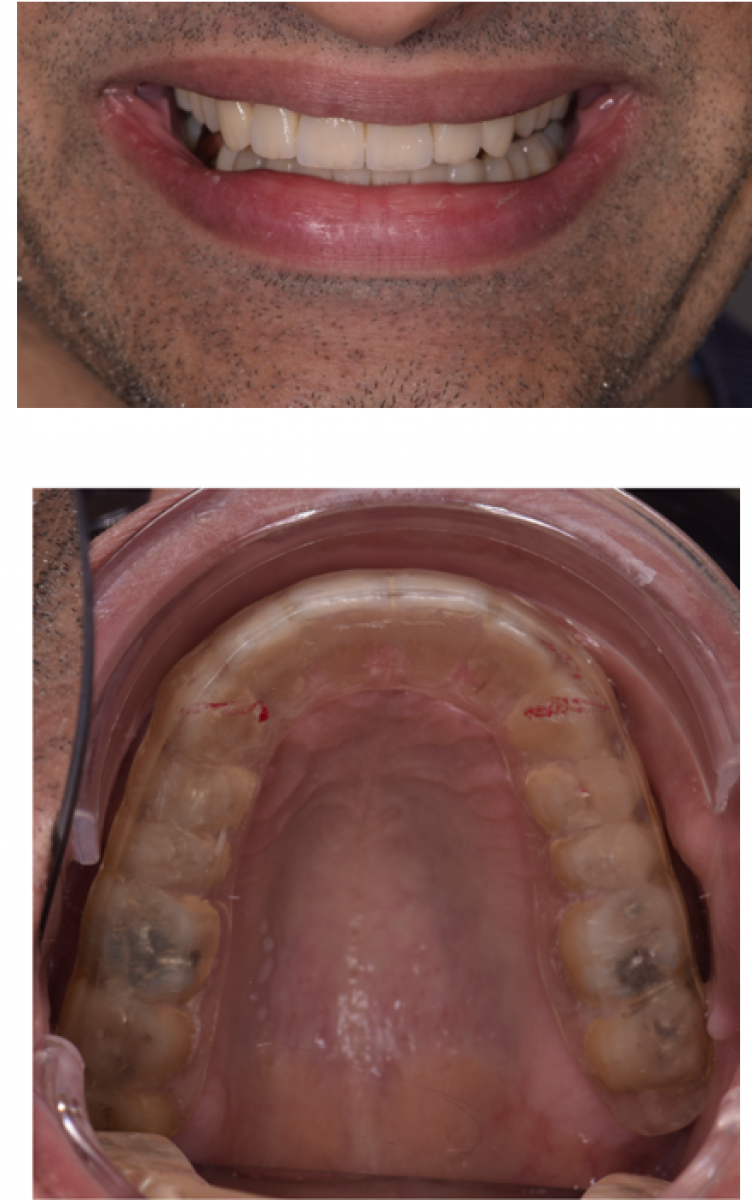
39-year-old male referred to improve aesthetics. His main concern was: ‘my teeth are not straight and are also chipping. UI do not want to have broken teeth’.
Findings:
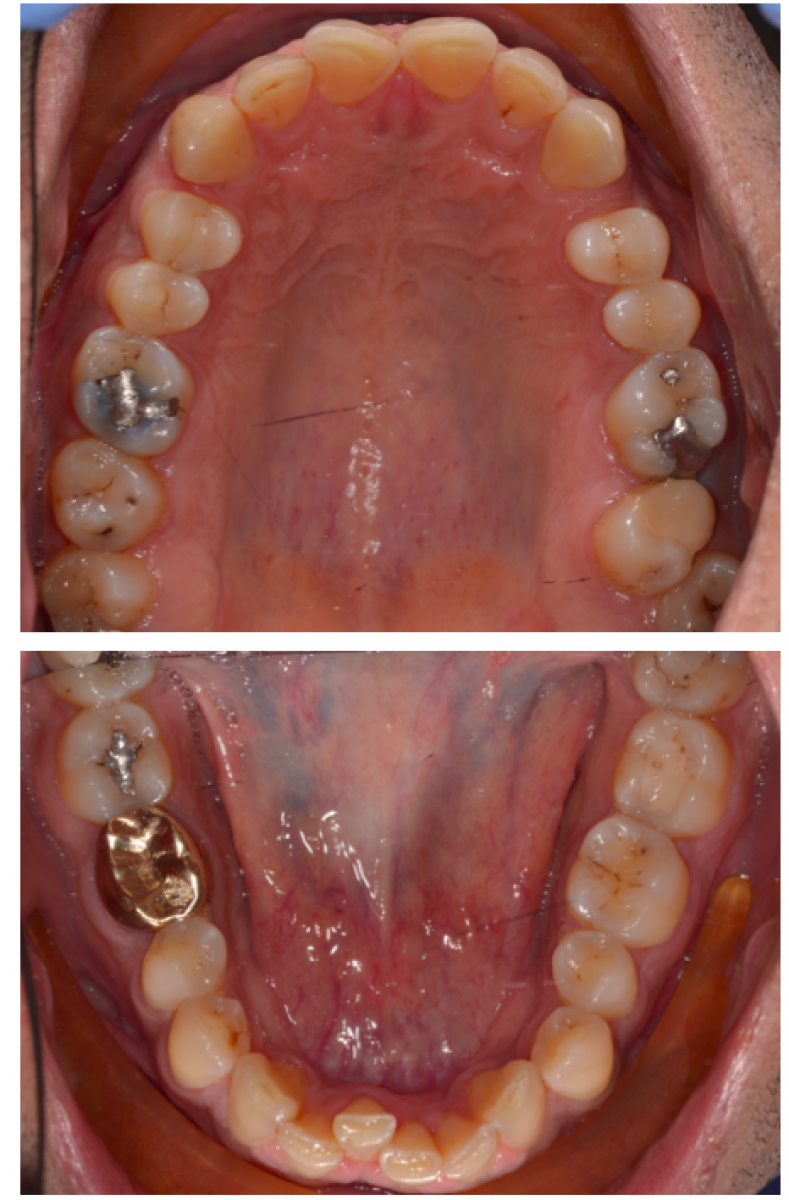
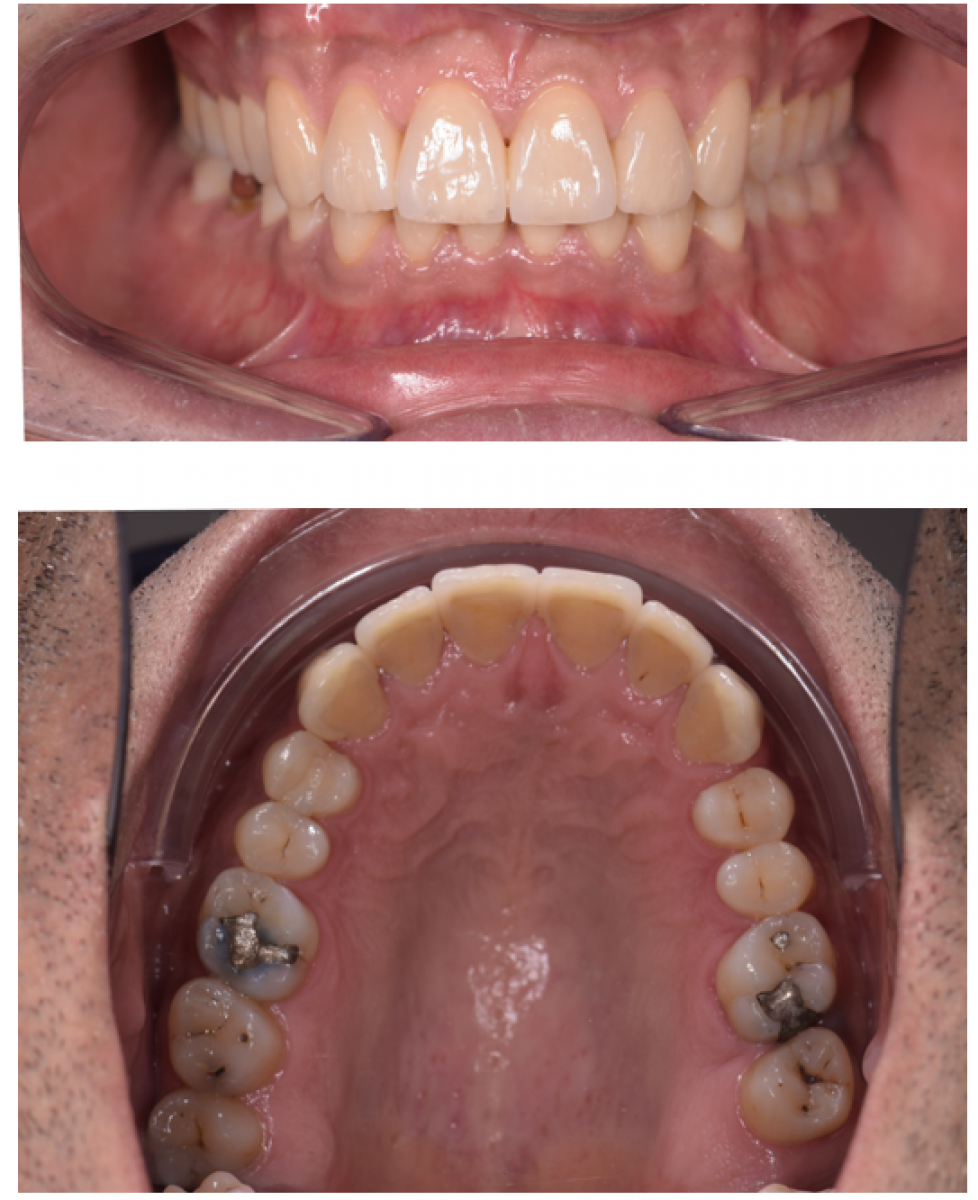
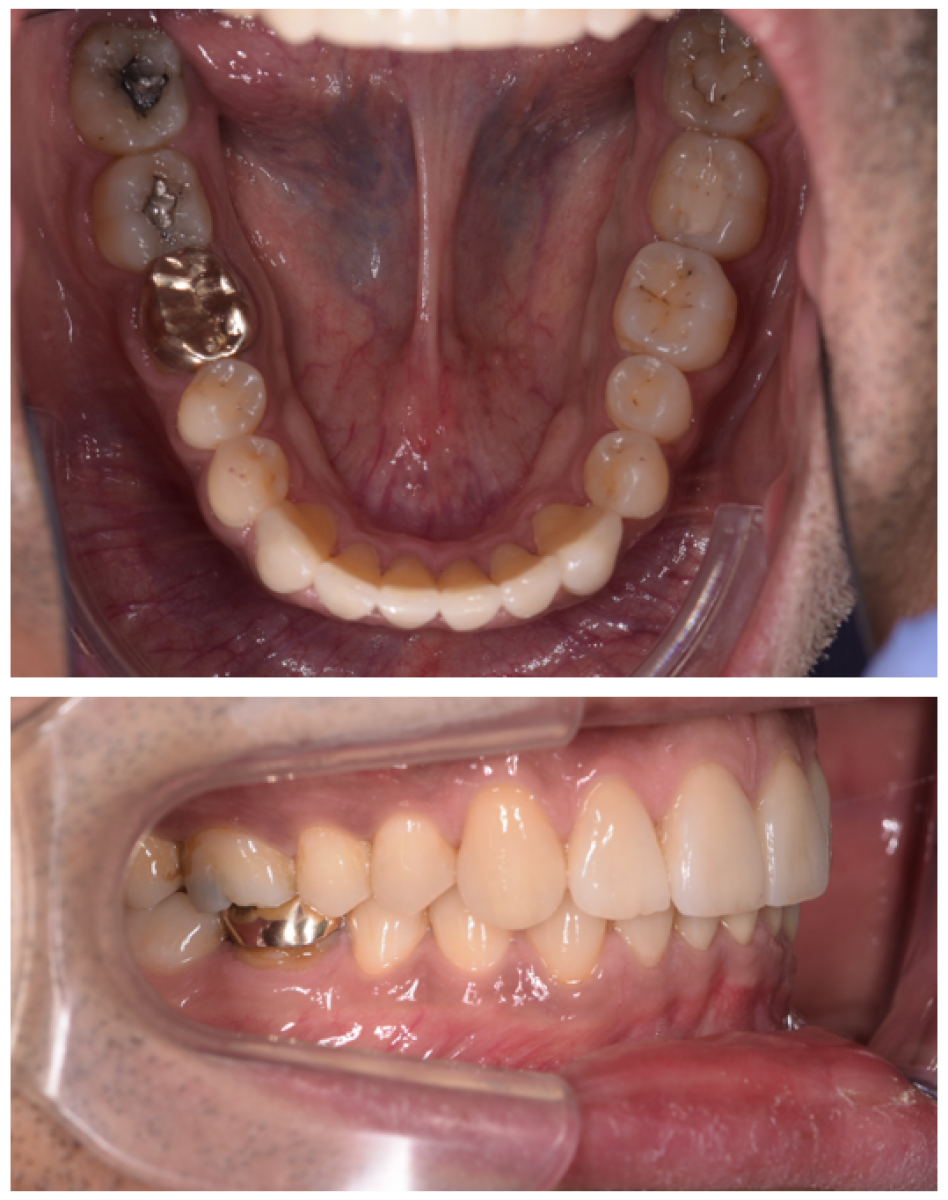
This patient had a non-excessive erosive diet. There was anterior TSL with a lack of anterior guidance. The patient had a stable CO-CR position. There was overclosure /deep bite with compensatory eruption of the upper central incisors and lower incisors. The skeletal pattern was class 2 due to a shorter mandible corpus on a low mandibular plane angle. This indicated strong closing muscles and heavy biting forces. There were upper spaces indicative of heavy forces and driving on the incisor’s forwards.
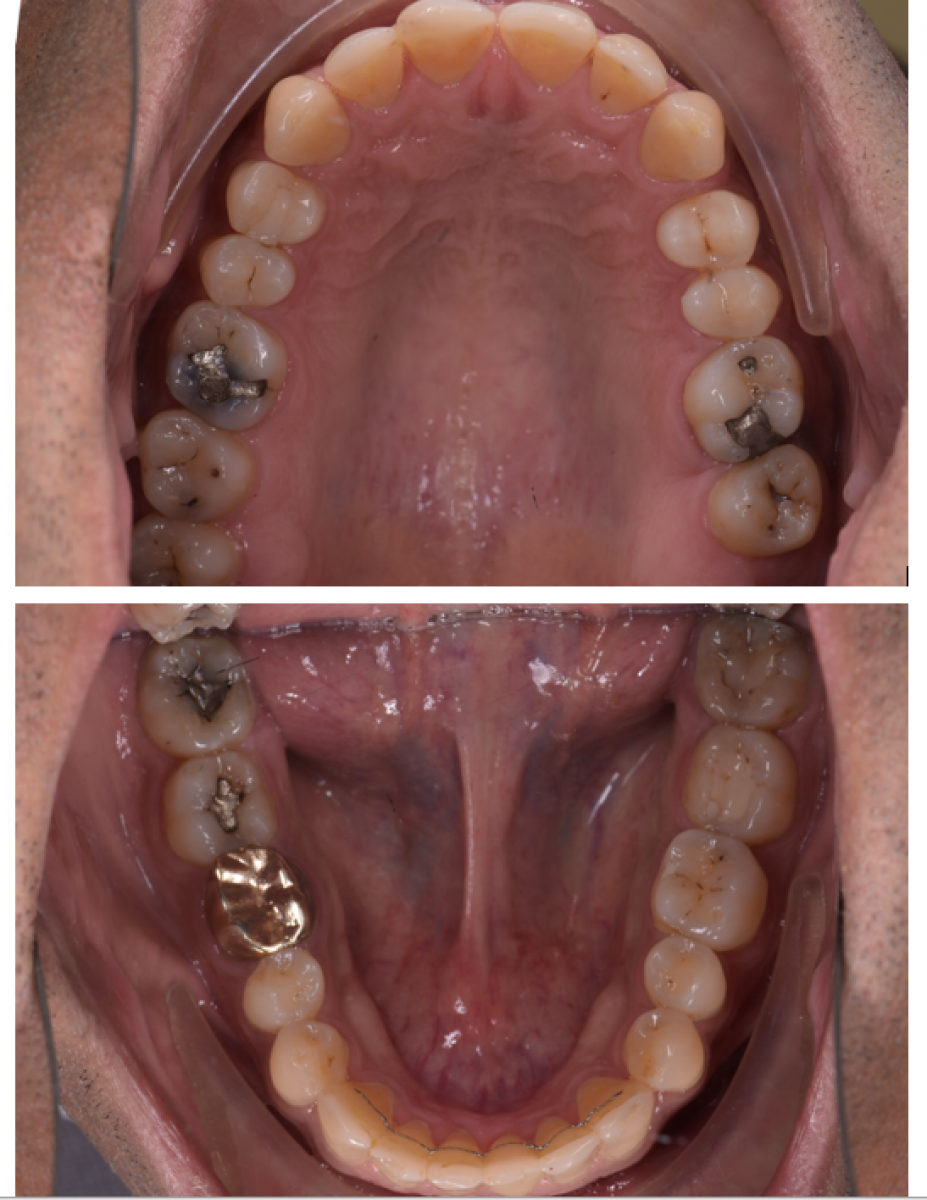
The upper left first and second molar were heavily restored. The upper left second molar had fractured twice and was in need of elective root canal treatment + full coverage restoration or extraction. All third molars were present.
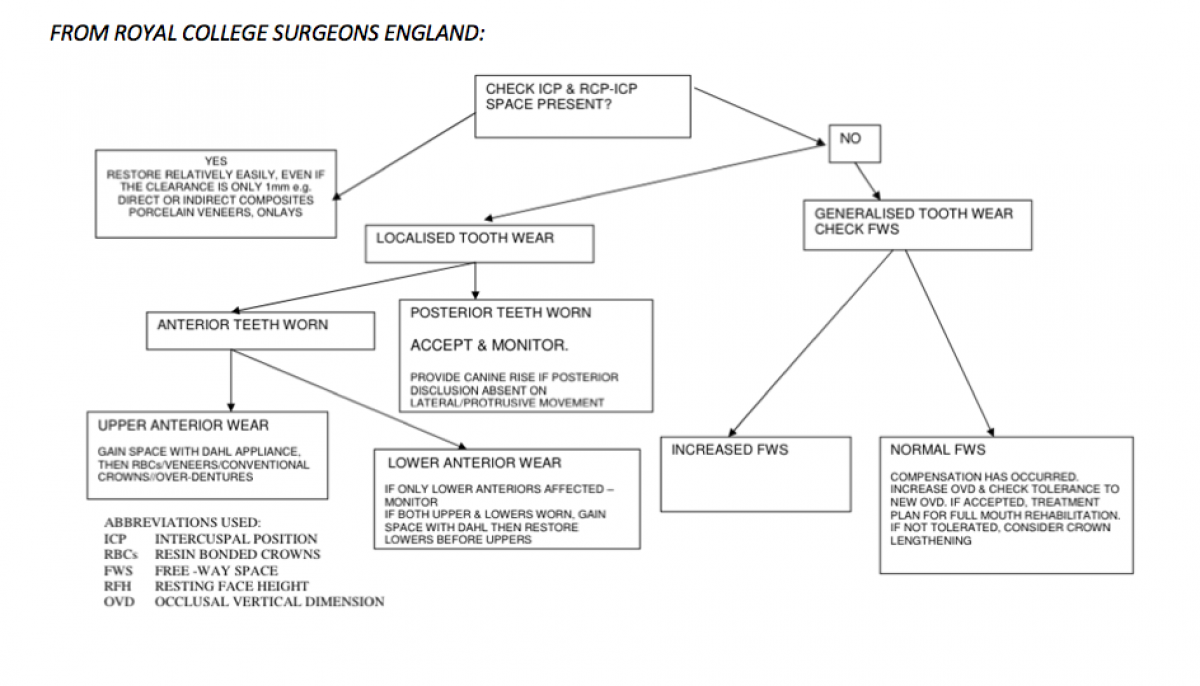
Treatment options:
1. Michigan splint and monitor TSL and occlusion.
2. Full mouth restorative solution with NO orthodontics
3. Orthodontic / Restorative solution (ideal)
After discussion with the restorative dentists and patient option 3 was chosen. We knew it would be a long treatment plan. The greater preservation of tooth structure in comparison to option 2 and the orthodontic mesial movement of the upper left wisdom tooth to replace the compromised upper left second molar were important considerations to the plan.
GOALS:
1. Alignment of dental arches.
2. Harmonise the gingival margins in the anterior segments.
3. Gain space to restore form and shape to the anterior teeth.
4. Negate the need for long term restorations on the upper left second molar by mesialising the third molar.
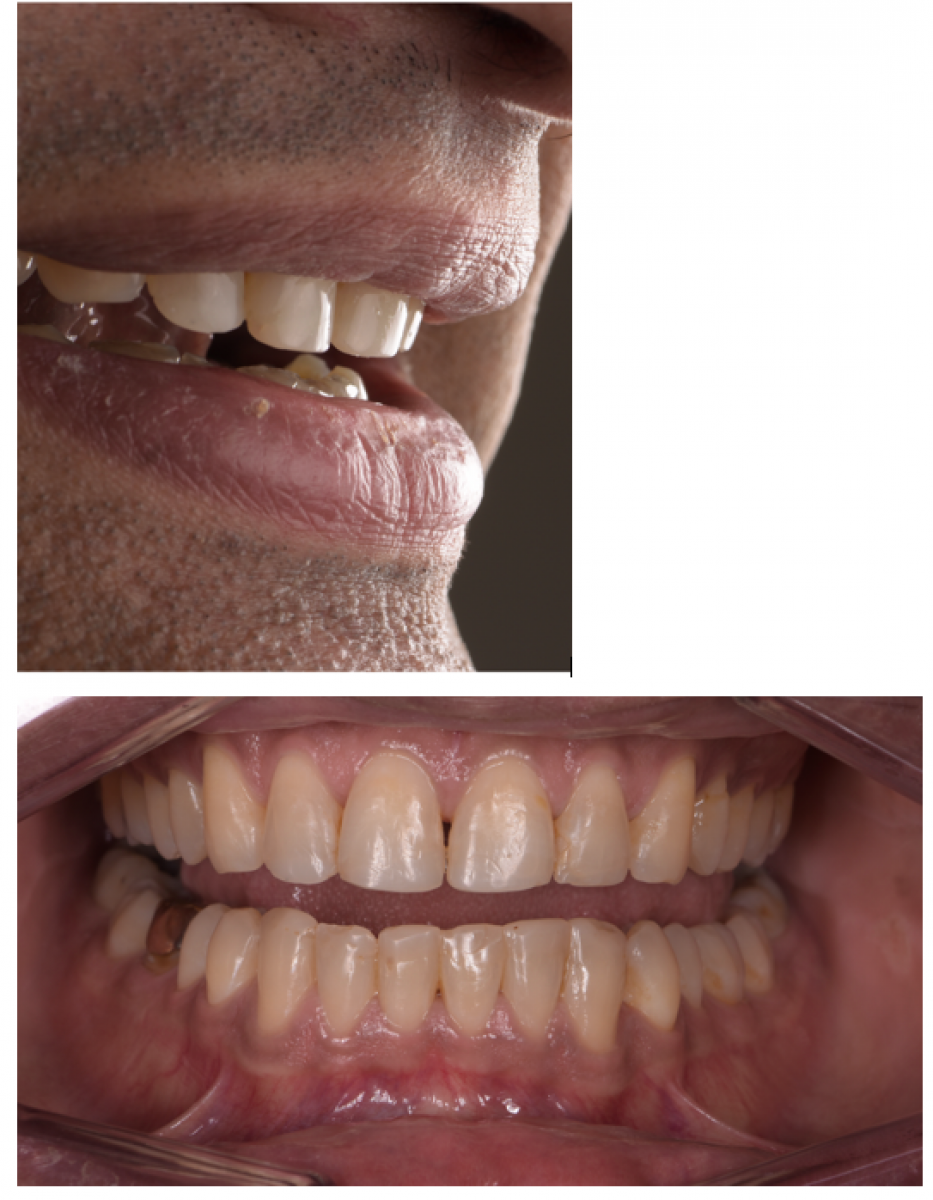
5. Provisional composite restorations on the anterior teeth to ensure proper aesthetics and functional stability.
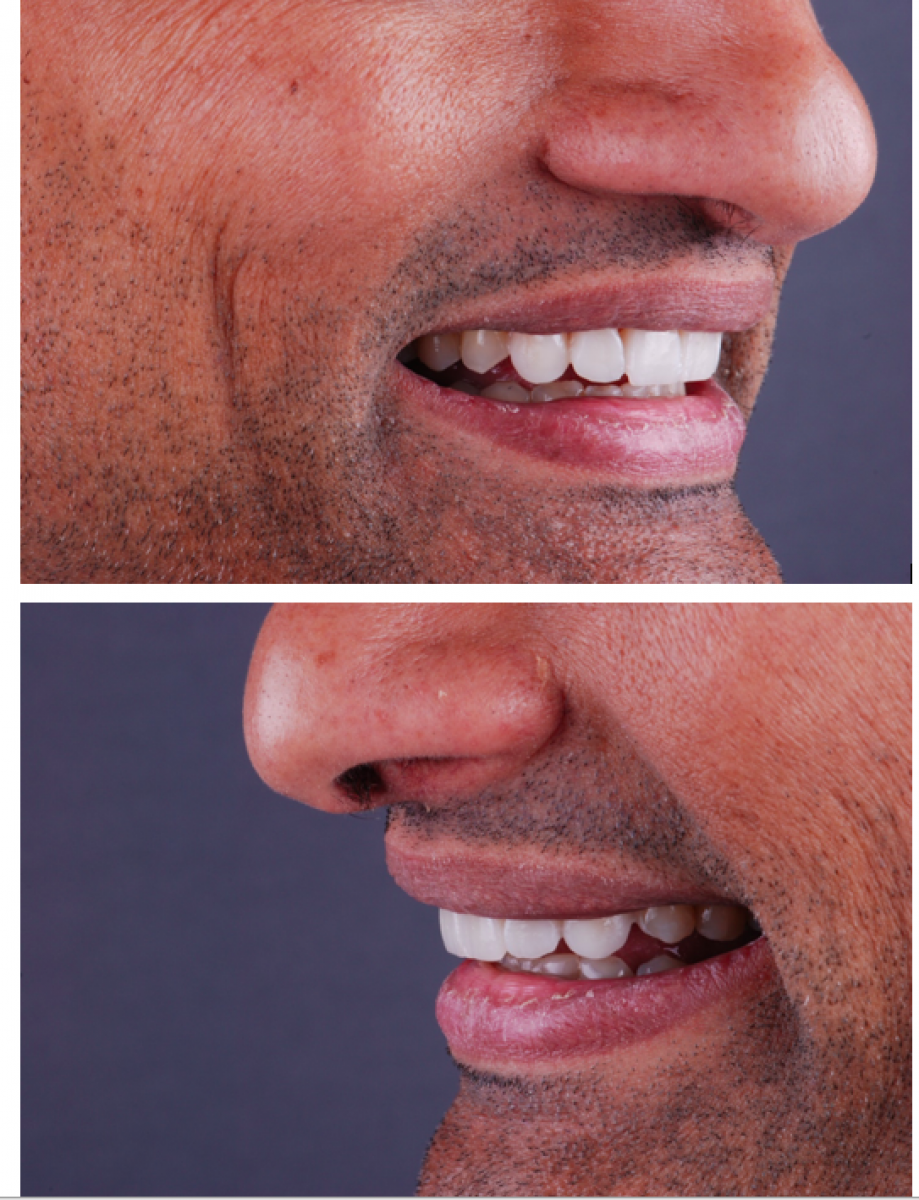
6. Definitive ceramic veneer restorations.
7. Maintenance with full coverage Michigan splint at night.
8. Eventual removal of remaining wisdom teeth.
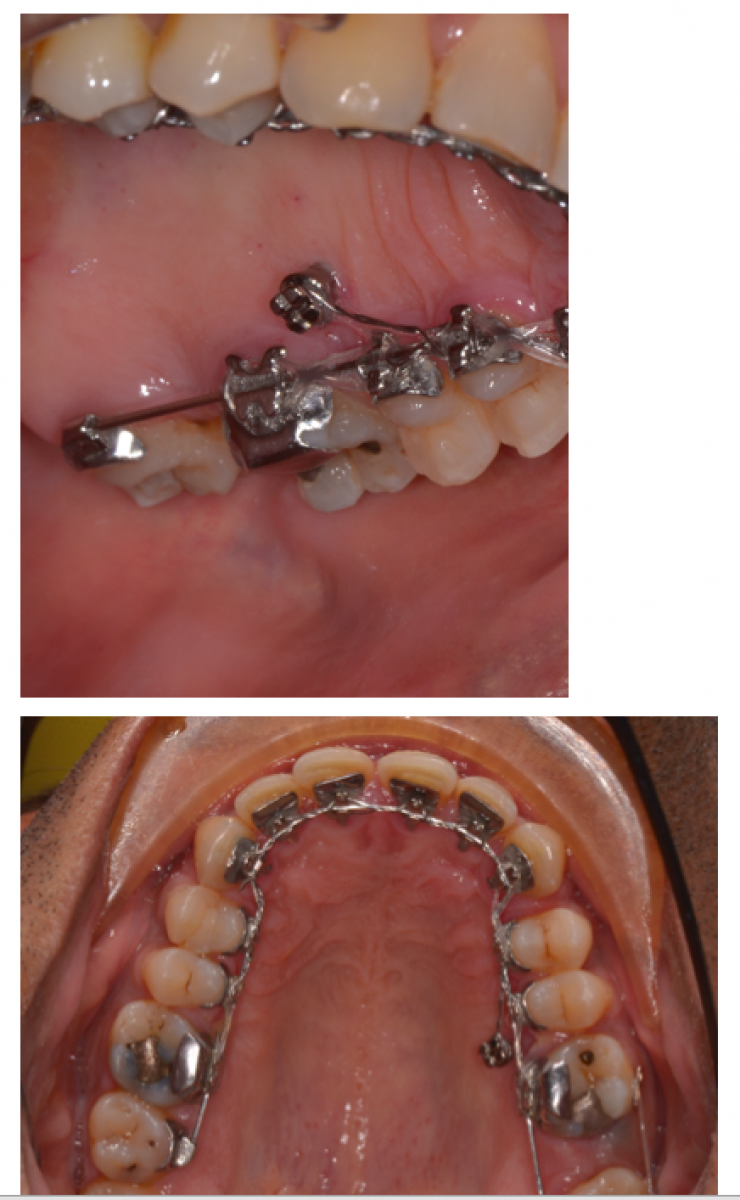
Mechanics:
1. Lingual bracing. The lower anterior teeth would contact on the palatal brackets of the upper incisors. This would have an automatic bite-opening effect and ‘dahl-like’ effect.
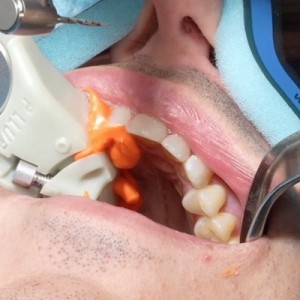
2. Extraction of upper left second molar. Palatal mini screw for indirect anchorage.
3. Removal of upper lingual braces for provisional composites.
4. Replacement of labial upper fixed appliances for finishing and detailing in the final 4 months.
5. Lower finished with lingual appliances.
Important points:
• Analyse the shape of TSL -it can tell you a lot about the cause of TSL.
• Gingival margins should be used as a reference for intrusion of worn teeth.
• Study the occlusal plane of the patient on a lateral cephalometric radiograph (ask the orthodontist for a copy). The relationship of the upper and lower anterior teeth in relation to the occlusal plane will can determine if the deep bite is caused by overeruption of the maxillary or mandibular teeth.
• Ensure patient has stable CO-CR position. De-program with a splint if required and re-evaluate the articulated models. (note some patients may be orthognathic mandibular advancement cases which are habitually posturing).
• The composite provisionals not only ensure proper shape, form and function but also boost the confidence and motivation of the patient in this lengthy treatment approach.
• Alveolar bone level of intruded teeth remains relatively constant relative to the cementoenamel junction, indicating bone follows the teeth during intrusion. There is however an average of 1.5mm apical root resorption following intrusion. This is important when considering future crown to root ratios.
Key points from this case:
• Treatment duration was 46 months overall. Patient compliance and motivation are fundamental in this multi-stage treatment.
• Extremely close collaboration with restorative dentist and orthodontist is key for the quality of outcome and patient experience. The effort is well worth it!
• Use provisional restorations to ensure form, shape and function and re-check CO-CR stability. Leave the patient with Provisionals for 4-6 months if possible, for the periodontal fibres to reorientate and stabilise.
• After the definitive restorations. Use a full coverage splint BUT see the patient regularly to check the splint and adjust accordingly.
Orthodontists: Dr Kaval Patel & Dr Carmen Costea
Orthodontist Therapists: Lisa Sheppard & Marge Kose
General Dentist: Dr Anand Gupta (composite Provisionals)
Restorative Specialist: Dr Pablo Pavon (definitive restorations)
Technician: Mr Inigo Casares
 Related articles
Related articles
Prosthodontics 18 May 2023
Evaluating the reliability of a new portable device to diagnose nocturnal bruxism
Bruxoff is a portable sleep bruxism assessment device that combines electromyography and heart rate assessment. In this study, authors investigated the reliability and validity of the device...
McEnhill’s father was a dentist and she said that she spent part of her teenage years working at his dental practice. “I learned very quickly how to work with patients in an extremely busy...
Dr. Andrea Shepperson talked about her background in dentistry and her new book, “Managing Tooth Wear,” available for pre-order in April 2023.
Prosthodontics 01 October 2022
Pilot study: 24 months in vivo wear of enamel antagonists to lithium disilicate implant crowns
To evaluate whether there is a significant difference between the ratio of wear of lithium disilicate implant crowns and their enamel antagonists and adjacent enamel or enamel antagonist contacts.
Digital Dentistry 23 October 2019
Wear of CAD-CAM ceramic single crowns and opposing natural teeth: glass matrix vs resin matrix
Contemporary computer-aided design and manufacturing (CAD/CAM) systems involve a wide range of dental restoration indications such as inlays, onlays, laminate...
 Read more
Read more
Dentistry Today recently attended a robotic-assisted dental implant procedure performed by Jay Neugarten, DDS, MD, FACS, utilizing the Yomi S robotic guidance s
Endodontics 21 April 2026
For a daily dental practice, the Panoramic (PANO) X-ray film is one of the most commonly used dental X-rays.
Editorials 21 April 2026
NYU Dentistry Receives $5M to Expand Oral Health Care for Children with Disabilities
State funding will create dedicated space for pediatric and adolescent care and improve access for people with disabilities across the lifespan