Open vs closed surgical exposure of palatally displaced canines
Davide Elsido
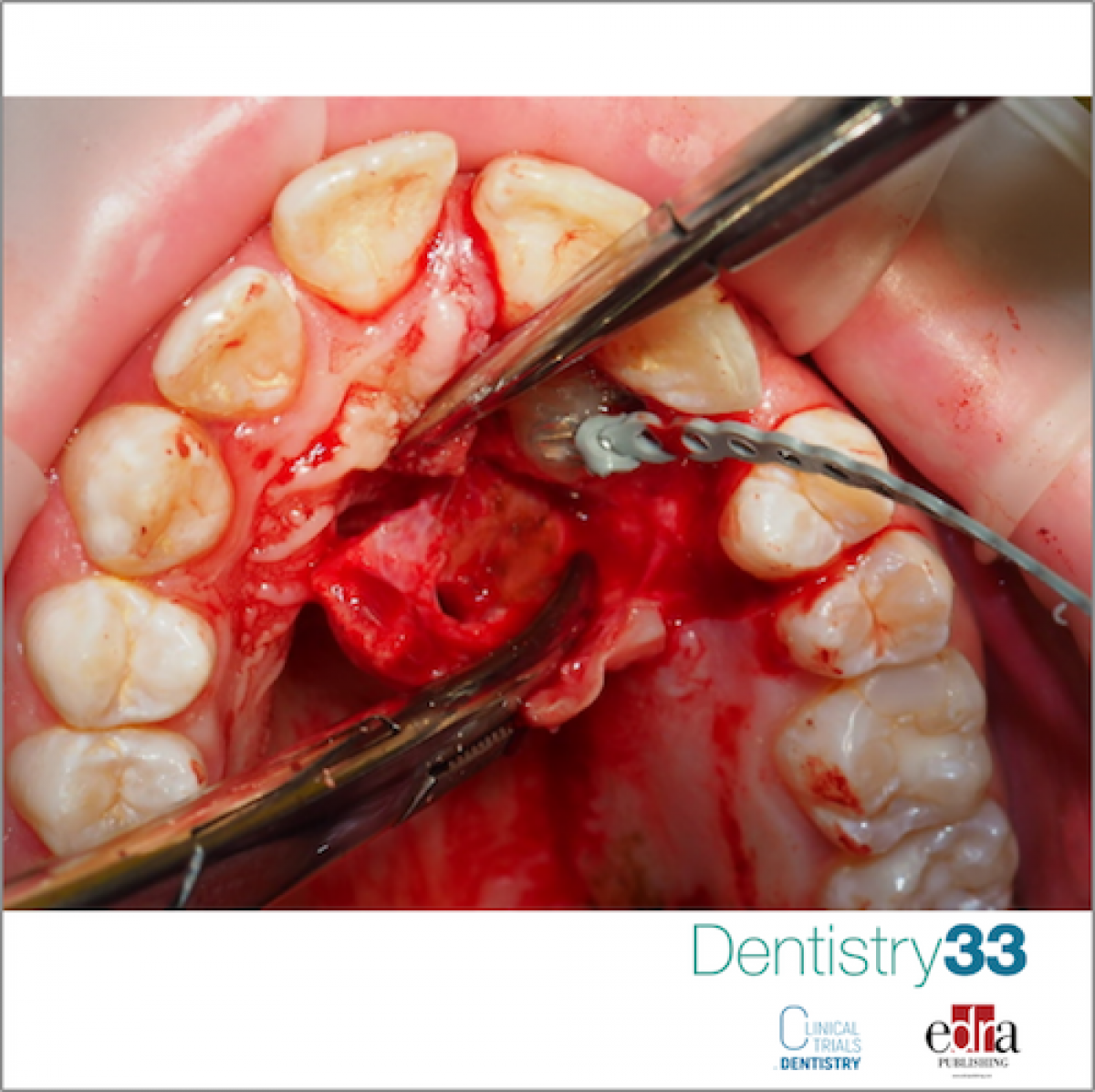
The treatment of palatal displaced canines (PDCs) is one of the most challenging treatments in orthodontic dental care. The invasive and long-lasting treatment often requires interceptive extraction of the deciduous canine at an early age, which might correct the eruption path of the PDC in 67%–69% of the cases. When interceptive treatment is unsuccessful, subsequent surgical exposure with following long-lasting orthodontic care is needed. The preferences for which of the two main surgical exposure techniques to choose, open or closed exposure, differ. The main difference between the techniques is whether the PDC is allowed to erupt spontaneously or if active orthodontic traction starts directly after surgery. In the open exposure technique, the palatal tissue is removed, and the canine is allowed to erupt spontaneously without any orthodontic traction until it erupts into the oral cavity. In the closed exposure, a chain is bonded to the PDC and the canine is orthodontically moved under the mucosa until eruption. The choice between the two current surgical techniques has been suggested to influence important outcomes such as patients’ perceptions of pain, eruption and treatment time and complications. Thereto, patients’ perceptions of invasive dental treatments may incorporate the risk of future dental anxiety, while prolonged orthodontic treatment time contributes to harmful side effects such as root resorption. These are important issues for both patients and their parents. In cases with several treatment options, the clinicians should choose the treatment that most benefits the patient. Inconsistency regarding treatment outcomes, with no consensus on which surgical technique benefits patients the most, leads to a need for randomized controlled trial.
This kind of RCT appeared on a recent issue of the European Journal of Orthodontics, comparing the outcomes of open and closed surgical exposure of PDCs.
Comparison of the two surgical exposure techniques, open and closed exposure, showed that: treatments were equally successful, with all PDCs aligned in their correct position in the dental arch; PDCs in the open exposure group erupted, in mean, 3 months faster, but the total treatment time was equal between the groups; the closed exposure group experienced more pain and discomfort during active orthodontic traction and consumed more analgesics; there were no indications of increase in dental fear levels, regardless of the surgical technique performed; clinical side effects in terms of root resorption or decreased root length did not differ between surgical exposure groups and group differences in periodontal status of the adjacent laterals were negligible and of no clinical relevance.
 Related articles
Related articles
Orthodontics 20 July 2022
The maxillary canines usually emerge at the mean age of 10.5 years in girls and 11.5 years in boys, with individual variation of 3–4 years. In 2–3 per cent...
 Read more
Read more
When patients brush their teeth before heading to bed, many assume their manual brush removes enough plaque.
News 14 May 2026
uLab Systems recently announced the promotion of three senior leaders into expanded roles across the company, reflecting their individual achievements and their consistent dedicati
News 14 May 2026
Reduces total funded debt by more than $1.1 billion, creating a more sustainable capital structure and better positioning DCA for future growth.
Editorials 14 May 2026
From California to Canada: CU Anschutz School of Dental Medicine at ADEA, GRC and IADR 2026
The CU Anschutz School of Dental Medicine will showcase a wide breadth of educational innovation, faculty development, clinical training and research at three major gatherings this
Oral surgery 14 May 2026
This peer-reviewed oral surgery article summarizes clinical evidence from International journal of oral and maxillofacial surgery (2025). It focuses on findings that may help dental professionals...