Innovative technique of peri-implant sub-periosteal bone thickening for the management of dehiscences in implantology
Lara Figini
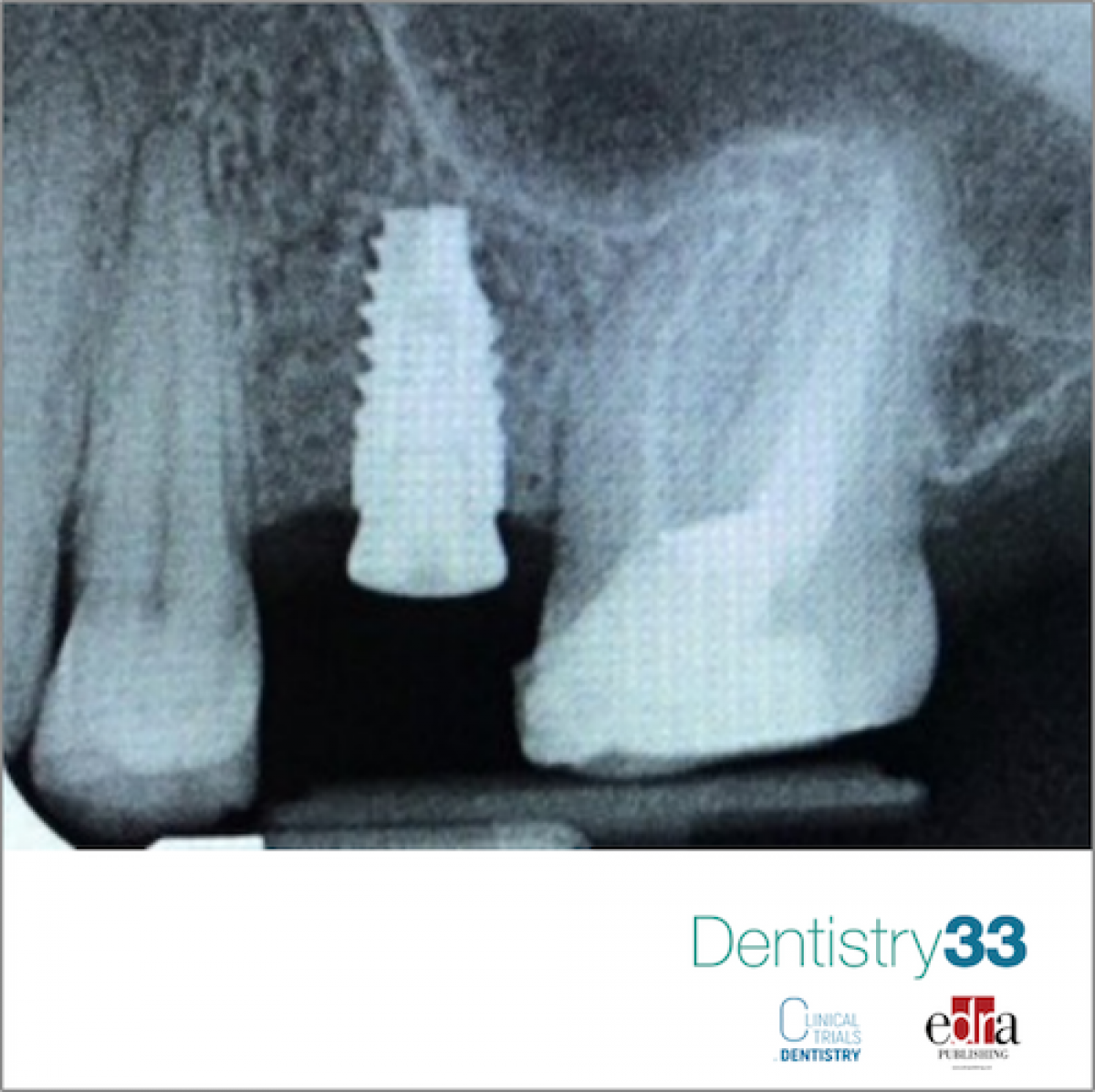
The placement of an implant where there is reduced bone thickness often results in peri-implant bone dehiscence or fenestration.
Even in the presence of intact but thin buccal cortical bone, implant placement can lead to vertical bone loss with exposure of the coronal part of the implant.
Recently Trombelli, Severi, Pramstraller, Farina and coll. (2018) proposed a simplified bone augmentation procedure, called Subperiosteal Peri-implant Bone Thickening Technique (SPAL), based on the use of the periosteum as a membrane / barrier and a graft as a "device" to create space for bone augmentation. concomitant with implant placement. In the study that we are going to summarize, the effectiveness of this technique was evaluated to correct peri-implant bone dehiscence and / or to increase the thickness of the peri-implant bone if necessary.
Materials and methods
In this Italian retrospective study by Trobelli et al., Published in Clinical Oral Implants Research 31-2020, the authors presented an innovative implant surgical technique where there was little or insufficient bone thickness (less than 2 mm) and evaluated the condition of the short-term peri-implant tissue by comparing the results obtained in patients in whom the SPAL technique (Sub-periosteal Peri-implant Augmented Layer or sub-periostal peri-implant bone thickening technique) was performed compared with the results obtained in patients with peri-implant buccal bone thickness adequate (≥2 mm) and treated with traditional method. Before implant placement, all patients included in the study underwent treatment for any carious lesions and periodontal diseases present. All surgical procedures were performed by two periodontal experts (L.T. and M.P.). Patients were given 2 g amoxicillin + clavulanic acid (Augmentin, GlaxoSmithKline) one hour before the surgery. Local anesthesia was achieved using articaine with 1: 100,000 adrenaline administered by local infiltration.
Two groups compared:
- SPAL group 1 or experimental (comprising the SPAL dehiscence subgroup + SPAL thin bone thickness subgroup) comprising patients in whom there was a dehiscence defect or a thin buccal peri-implant bone thickness (PBBP) corrected with the SPAL technique performed simultaneously with the positioning of the 'plant.
- Group 2 or control group including patients treated in the traditional way as having a residual buccal peri-implant bone thickness (PBBP) ≥2 mm at the time of implant insertion. As a primary outcome, the number of peri-implant sites positive for bleeding on probing (BoP) at 6 months after prosthetic loading was evaluated. As secondary outcomes, the height of the keratinized mucosa (KM), the level of marginal soft tissues, the plaque index, the depth of peri-implant probing (PD), suppuration on probing were evaluated. Radiographic bone level (RBL) was also assessed.
SPAL technique:
A flap was performed and the periosteal layer was lifted from the bone and the sites for the accommodation of the implants were prepared. If buccal dehiscence was evident, or buccal bone thickness was too thin (less than 2mm), a deproteinized xenograft of bovine mineral origin was performed at the same time (Bio-Oss® spongy granules, particle size 0.25-1 , 0 mm; Geistlich Pharma, AG) alone or in combination with autologous cortical bone particles and the periosteal layer was sutured to the oral flap. The buccal dehiscence was completely corrected. A free gingival graft was used to obtain adequate dimensions of peri-implant keratinized mucosa. Clinical and radiographic checks were conducted 6 months after the delivery of the prosthesis.
Surgical procedures - control group:
A full thickness buccal and lingual / palatal flap was lifted to expose the bony crest. The implant site was prepared according to the manufacturer's directions and implants were placed and since there was a PBBP thickness ≥2 mm in these patients, no bone augmentation procedures were performed.
Postoperative procedures in all patients:
Patients were instructed not to wear removable prostheses to avoid compression on the surgical site for at least 4 weeks and not to use while chewing or brushing the treated area for about 2 weeks. Rinses with chlorhexidine 0.12% (Curasept ADS Regenerating Treatment®; Curaden Healthcare) for 3 weeks. The sutures were removed 2 weeks after surgery. Prosthetic rehabilitation was started 3-4 months after implant placement in the control group and at least 4 weeks after implant reopening in the SPAL group.
Results
Thirty-four patients (11 in the SPAL dehiscence group, 11 in the SPAL thin thickness group and 12 in the control group) were included. In each SPAL subgroup 10 patients (90.9%) showed a peri-implant tissue thickness ≥2 mm in the most coronal portion of the implant. The prevalence (number) of BoP-positive sites was 2, 1, and 0 in the SPAL dehiscence, SPAL thin bone thickness, and control groups, respectively. RBL amounted to 0.3 mm in the SPAL dehiscence subgroup, 0.2 mm in the thin thickness SPAL subgroup and 0 mm in the control group.
Conclusions
From the data of this study, which must be confirmed in other similar studies, it can be concluded that after 6 months of prosthetic loading, patients treated with the SPAL technique show limited inflammation of the peri-implant mucosa in association with adequate superficial PD and KM. In implants that received the SPAL technique, however, the interproximal radiographic bone level (RBL) was found to be more apical than its ideal position.
Clinical implications
Given that favorable short-term results have been observed using the SPAL technique, it is possible to hope for good results even in the long term from this technique. However, further long-term studies are needed to confirm.
For additional information: Peri-implant tissue conditions at implants treated with Sub-periosteal Peri-implant Augmented Layer technique: A retrospective case series
 Related articles
Related articles
Dentistry Today recently attended a robotic-assisted dental implant procedure performed by Jay Neugarten, DDS, MD, FACS, utilizing the Yomi S robotic guidance system .
Implantology 22 April 2026
To update in new biopolymers and innovations for ocular prostheses and visual implants for visual care.
Dentistry Today recently attended a robotic-assisted dental implant procedure performed by Jay Neugarten, DDS, MD, FACS, utilizing the Yomi S robotic guidance s
Endodontics 21 April 2026
For a daily dental practice, the Panoramic (PANO) X-ray film is one of the most commonly used dental X-rays.
 Read more
Read more
Salt Lake City, Utah— The Monet+ laser curing light represents a significant advancement in laser curing technology.
News 21 May 2026
Through strategic participation at AAO 2026, Graphy strengthens its global footprint by delivering scalable SMA solutions and a unified digital platform to the North American ortho
News 21 May 2026
Recognizing More Than 20 Years of Giving Back Through Charitable Services to Help Spread Smiles
As the University of Colorado School of Dental Medicine celebrates the graduating DDS Class of 2025, we are proud to recognize the students and faculty members whose exceptional de
Orthodontics 21 May 2026
This peer-reviewed orthodontics article summarizes clinical evidence from PloS one (2026). It focuses on findings that may help dental professionals evaluate treatment decisions, patient outcomes, or...