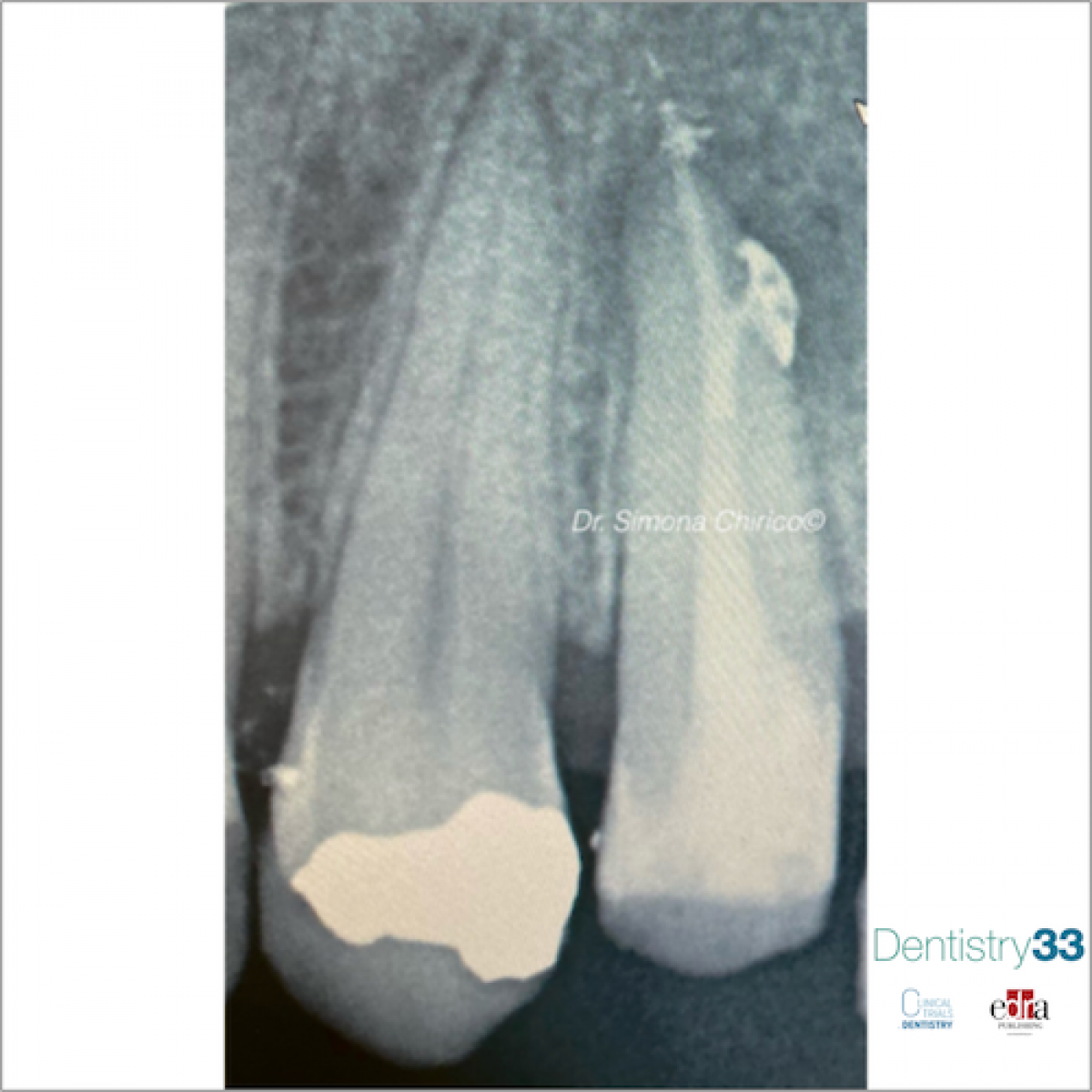
Complex endodontic treatments: what interferes with their long-term success?
Lara Figini
After root canal treatment (primary or secondary treatment), the prognosis for endodontic healing is influenced by several factors:
- Root anatomy
- The quality and adequacy of the endodontic therapy performed
- the presence of a preoperative radiolucency,
- the development of complications during the operative phases (for example broken instruments or perforations),
- the quality of the coronal restoration,
- the quality of the root canal filling
- the preservation of the original morphology of the root canal etc.
Not all root canal therapies are the same, but they have different levels of difficulty depending on the root anatomy, previous treatments performed, etc.
To assess the difficulty of endodontic treatment, guidelines for the dentist have been developed which are based on an endodontic treatment classification score (ETC), with the primary purpose of helping the general practitioner when referring a patient to one. endodontic specialist or not.
The ETC scale divides the level of difficulty of endodontic treatment into three classes.
- Class I indicates an endodontic treatment of medium risk, with limited preoperative problems (for example a molar tooth with 3 canals without calcifications or root curvatures, easy to isolate with the rubber dam).
- Class II represents a high risk of possible complications during the endodontic procedure so obtaining a predictable treatment outcome would be difficult even for an experienced dentist (e.g. a molar tooth with> 3 canals, moderate root curvature (10◦-30 ◦) and calcified canals).
- Class III, includes high-risk root canal treatments with procedural complications and for which advanced knowledge and specific tools are required to obtain a predictable treatment result (for example a molar tooth with the presence of a broken instrument).
Materials and methods
In a clinical study, published in the February 2021 Jornal of Dentistry, the authors assessed the survival and success of molar teeth with ETC scores of II and III, after complex endodontic treatment, with up to 89 months of follow-up. Endodontically treated maxillary and mandibular first and second molars between January 2011 and October 2017 were included in the study. A total of 416 root canal treatments were performed by two experienced dentists. The inclusion criteria were: molar teeth requiring primary or secondary root canal treatment, patients over the age of 18 and with an American Society of Anaesthesiologists (ASA) score of ≤2. Teeth with open apices, in which non-surgical treatment combined with surgical treatment was performed, with an ETC score of 1 or patients younger than 18 years or with an ASA score> 2 were excluded. The quality of the restoration was assessed using the FDI criteria. All endodontic procedures were performed under the microscope (OPMI Pico; Zeiss, Oberkochen, Germany) with rubber dam isolation and according to a standardized operating protocol.
Results
279 endodontically treated molars in 245 patients were included for survival analysis and 268 molars for endodontic success. After 89 months, cumulative survival was 91.7% [95% CI: 86.8% –94.9%]. The absence of adjacent teeth and the alteration in the morphology of the root canal significantly reduced the probability of survival of the treated teeth. Cumulative endodontic healing rates after 48 and 89 months were 82.2% and 51.1%, respectively. The alteration in the morphology of the root canal and the inadequate coronal seal significantly reduced the probability of endodontic healing. Indirect restorations achieved aesthetic results and biological FDI scores, however no significant difference was found between direct and indirect restorations with regards to functional FDI score.
Conclusions
From the data of this study, which must be confirmed in other similar studies, it can be concluded that after 89 months, the cumulative survival of molars requiring complex endodontic treatment is 91.7%.
For additional information: Survival of molar teeth in need of complex endodontic treatment: Influence of the endodontic treatment and quality of the restoration
 Read more
Read more
News 08 May 2026
Maria Gutierrez in Yorba Linda, California, has added the DEXIS Orthopantomograph OP 3D EX cone beam computed tomography (CBCT) system to its practice.
News 08 May 2026
35-year healthcare veteran who scaled dental and Medicaid programs to over $1 billion in revenue joins as LightSpun enters critical growth phase on the heels of NationsBenefits and
Dean Denise Kassebaum, DDS, MS, opened the University of Colorado School of Dental Medicine White Coat Ceremony with congratulations, appreciation and support for the DDS Classes o
Oral surgery 08 May 2026
This peer-reviewed oral surgery article summarizes clinical evidence from International journal of oral and maxillofacial surgery (2026). It focuses on findings that may help dental professionals...