Pterygoid implants in severe maxillary atrophy
Lara Figini
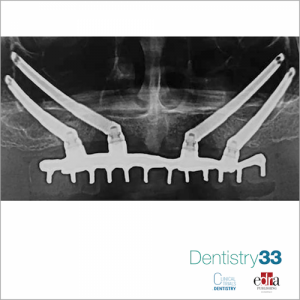
When bone volume is insufficient for implant placement, bone regeneration techniques can be used or the insertion of particularly inclined implants or zygomatic implants. The survival of implants placed in the posterior maxilla is dependent on the biomechanical characteristics of bone around the implant as high occlusal forces are developed in the molar region during mastication. These forces can also induce prosthetic complications, including fracture of the prosthesis, fracture of the screw and bone loss, especially when cantilevered prostheses are provided. The pterygomaxillary area has tended to never be much considered as a region suitable for implant placement. This region is often associated with both extensive bone degeneration (poor bone quality) and a reduced amount of cortical bone. In 1989, Tulasne8 described a method for inserting and engaging pterygoid implants in the cortical bone formed by the posterior wall of the maxillary tuberosity, horizontal process of the palatine bone, and pterygoid process of the sphenoid bone. Pterygoid implants are attractive because of the availability of dense cortical bone for engagement of the implant. They also help to
overcome the need for maxillary sinus lift or grafting procedures, reducing treatment time and allowing immediate loading of the implant. In addition, pterygoid implants allow the prosthesis to have sufficient posterior extensions, eliminating the need for distal cantilevers. Disadvantages of pterygoid implants include:
- the difficulty of the procedure which requires a certain learning curve for the surgeon,
- Proximity to vital anatomical structures e
- The difficulty of access for surgeon and patient.
Furthermore, it is difficult to radiographically assess the marginal bone loss around these implants.
Materials and Methods
In an Italian study, published on Journal of Prosthetic Dentistry, July 2021, the authors investigated the 1-year survival and success rates of pterygoid implants and prostheses in patients with severe posterior maxillary atrophy who required immediate fixed prosthesis for full arch. Fifteen participants were enrolled in the study, completely edentulous or with limited dentition in the maxillary arch and with severe atrophy of the posterior maxilla. Implant survival data were assessed at abutment connection time by mobility testing for each implant. After the placement of the prosthesis, survival was assessed by maintaining the marginal bone through panoramic radiographs, and the absence of pain or symptoms of infection was recorded. The t-test was used to assess the age difference between men and women (a = .05). Correlations between categorical variables (Fisher's exact test) were used to evaluate the possible association between the number of implants and the patient's age and the presence of comorbidities (a = .05)
Results
During the 1-year follow-up, high stability of the prosthesis and no loss of implants was observed for all participants. No patient reported any pain or paraesthesia. No peri-implant radiolucency was detected in the panoramic radiographs. The survival and success rates in the follow-up period were 100%.
Conclusions
From the data of this study, which must be confirmed in other similar studies, it can be concluded that:
1. Pterygoid implants offer a high success rate with little or no short-term complications.
2. The present study reported reliable results and accurate data on the survival and success rates of pterygoid implants.
3. New survival studies of pterygoid implants are needed with follow-up longer than 1 year.
Clinical implications
Based on the short-term clinical outcome of this study, surgeon should consider the insertion of pterygoid implants in patients with severe maxillary atrophy and consider them a predictable treatment option. Patient compliance before and after surgery is the key to implant survival. The data may lay the foundation for improved management of patients with severe posterior maxillary atrophy.
For additional information: Immediate fixed rehabilitation supported by pterygoid implants for participants with severe maxillary atrophy: 1-Year postloading results from a prospective cohort study
 Read more
Read more
New initiative invites dentists to experience DEXIS’ most advanced AI yet, built on scale, speed, and clinical trust.
News 05 June 2026
(Nasdaq: ALGN), a leading global medical device company that designs, manufactures, and sells the Invisalign® System of clear aligners, iTero™ intraoral scanners, and exocad™ CAD/C
News 05 June 2026
(Nasdaq: HSIC), the world’s largest provider of health care solutions to office-based dental and medical practitioners, today announced that its Board of Directors has elected Will
As the University of Colorado School of Dental Medicine celebrates the graduating DDS Class of 2025, we are proud to recognize the students and faculty members whose exceptional de
Oral surgery 05 June 2026
This peer-reviewed oral surgery article summarizes clinical evidence from International journal of oral and maxillofacial surgery (2026). It focuses on findings that may help dental professionals...