Use of 3D printed replica for autotransplantation: case report
Authors: Luigi Tagliatesta, Nadim Oliva, Giacomo Moretti, Alberto Scagnelli, Thomas Gaglione, Andrea Oliveira
Autologous dental transplantation is defined as the movement of a tooth from one alveolus to another, within the same person. The indications for performing an autotransplantation are mainly linked to agenesis, trauma and teeth severely compromised by caries. The most important success factors in dental autotransplantation are the correct preservation of the periodontal ligament (PDL) of the donor tooth and its correct adaptation in the recipient site.
In this clinical case, we present how complications of PDL as a result of excessive extra alveolar time or related to iatrogenic mechanical damage can be reduced thanks to diagnostic technologies like Cone Beam Computed Tomography (CBCT) and the creation of a three-dimensional model of the donor tooth through Computer Aided Design/Computer Aided Manufactoring processes (CAD / CAM).
A 22-year-old ASA I patient came to our attention.
During the visit we found a decayed upper first molar (2.6). We deemed it as irrecoverable. We observed the ipsilateral upper third molar (2.8) in excellent health without caries, endodontic and periodontals issues. Furthermore, 2.8 had not any occlusal contact due to the absence of the antagonist molar.
The young age of the patient, associated with a precarious economic condition, precluded prosthetic or implant-prosthetic therapies. Autotransplantation of 2.8 in 2.6 socket was indicated in this clinical case.
After extracting the DICOM sections of 2.8, an STL file could be developed through specific software. Finally, using a 3D printer, the 2.8 stereolithographic replica was created in a 1: 1.
The surgery was carried out with a clean preparation. We then carried out the following surgical maneuvers: local anesthesia, subperiosteal detachment, dislocation and avulsion of 2.6, revision of the alveolar socket, irrigation with physiological solution, alveoloplasty maneuvers guided by the 3D model using piezoelectric device and atraumatic avulsion maneuvers of 2.8.
The donor third molar was reduced in its occlusal contacts with the antagonist tooth (positioned outside the occlusion) and it was finally stabilized by a horizontal mattress suture using a 4/0 polyglycolic acid suture.
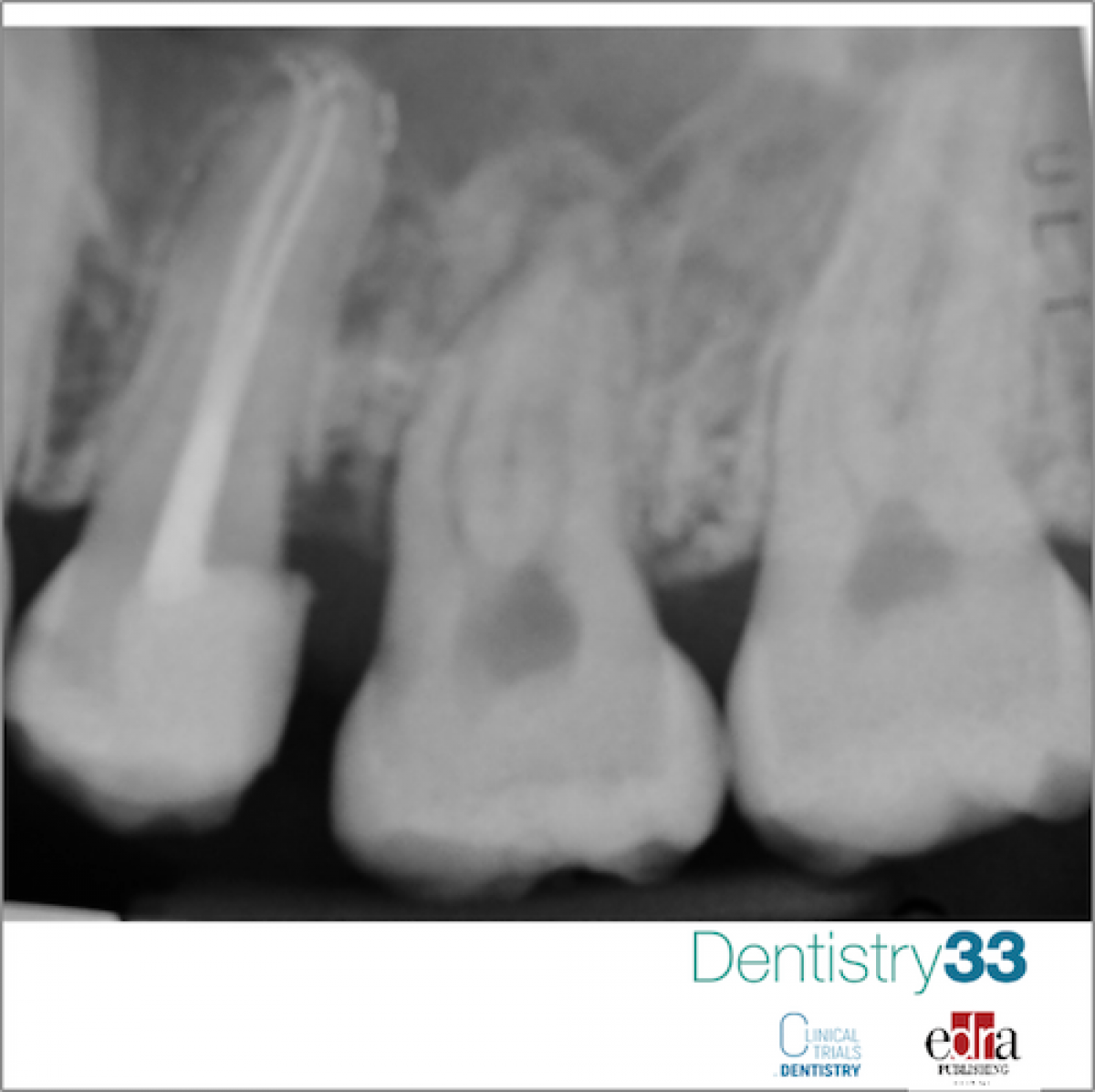
After a week, excellent clinical soft tissue healing was evidenced. Both the subsequent follow-up (after 2 and 6 months) reported a positive result for the pulp vitality of the donor tooth. After 8-month follow-up, a clinical check was performed and an intraoral x-ray of the autotransplanted tooth was performed (2.8): neither symptoms nor pathological signs of the dental or periodontal tissues were communicated or detected.
The use of a 3D replica has been shown to be useful in the dental autotransplantation procedure, especially by reducing the extraoral time of the PDL, the duration of surgical procedures and the iatrogenic trauma to the periodontal ligament, therefore increasing long-term success rates.
3D replica of donor teeth allows to periodontal ligament to stay healthy, improving the prognosis of autotransplanted teeth.
 Read more
Read more
New initiative invites dentists to experience DEXIS’ most advanced AI yet, built on scale, speed, and clinical trust.
News 05 June 2026
(Nasdaq: ALGN), a leading global medical device company that designs, manufactures, and sells the Invisalign® System of clear aligners, iTero™ intraoral scanners, and exocad™ CAD/C
News 05 June 2026
(Nasdaq: HSIC), the world’s largest provider of health care solutions to office-based dental and medical practitioners, today announced that its Board of Directors has elected Will
As the University of Colorado School of Dental Medicine celebrates the graduating DDS Class of 2025, we are proud to recognize the students and faculty members whose exceptional de
Oral surgery 05 June 2026
This peer-reviewed oral surgery article summarizes clinical evidence from International journal of oral and maxillofacial surgery (2026). It focuses on findings that may help dental professionals...